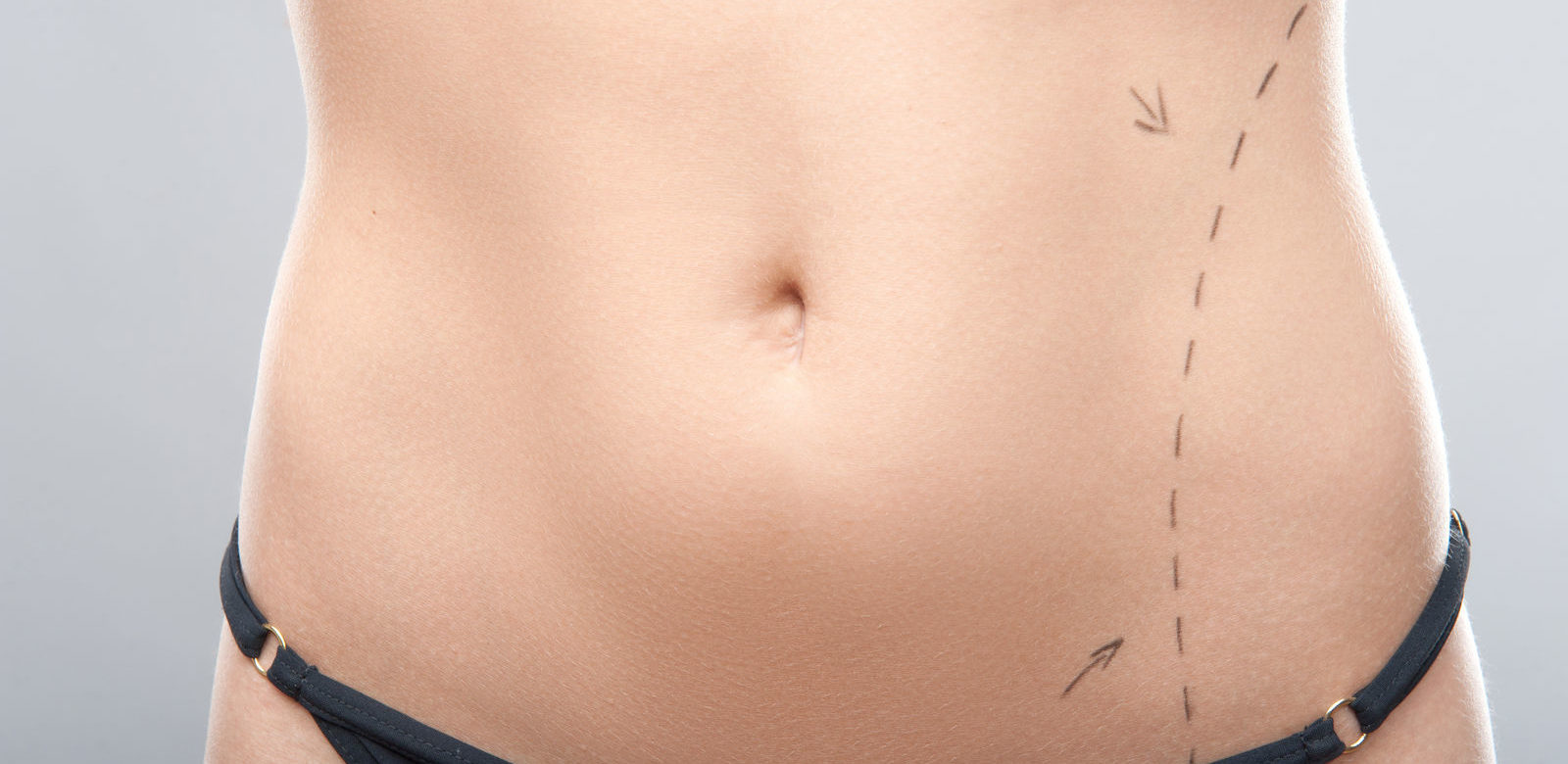
Is liposuction ever covered by health insurance?
“To sum it up…”
- Liposuction is a cosmetic procedure. Cosmetic procedures are not typically covered by insurance companies, Medicaid or Medicare
- There are some instances where insurance may cover liposuction. Liposuction as a treatment for lipomas, as part of a breast reduction or as part of a larger reconstructive surgery is often covered
- Call different insurance companies to compare their policies on using liposuction as a therapy in the treatment of disease
The obesity epidemic is widely cited as a leading cause of chronic disease and death in the United States. Even more worrisome is the rising prevalence of individuals with excess visceral fat, or the deep layer of fat that covers the abdominal organs. This type of fat is firm to the touch, difficult to lose and puts an individual at a high risk or mortality and morbidity. Liposuction is one way to remove the visceral layer of fat that covers the abdominal organs.
Less invasive than bariatric surgeries like the gastric sleeve and gastric bypass, liposuction is beneficial for individuals with normal or slightly higher than recommended body weight who carry a significant amount of visceral fat. For men, that means having a waist circumference larger than 40 inches. For women, the criteria to assign risk is a waist circumference of 35.
Understanding the benefits of liposuction, the question becomes, does insurance ever cover liposuction? The answer, like most answers to insurance questions, is complicated and depends on the type of insurance a patient has. Read on to discover more about liposuction as it relates to insurance coverage, both private and public.
Also, be sure to enter your zip code on our page before you leave to compare health insurance providers and policies free of charge!
When is liposuction deemed medically necessary or therapeutic?

The sad fact is that, usually, liposuction is not covered by insurance. That is because liposuction is considered a cosmetic procedure most of the time. Cosmetic procedures are, by their very nature elective, and patients typically must pay out of pocket for this type of medical care.
Insurance in the United States is meant to operate as cost sharing and risk sharing between the individual and the insurance company as well as between the individual and other individuals in their insurance pool.
Elective procedures cannot factor into this model. Consider the implications of everyone in an insurance pool electing to have cosmetic surgeries like rhinoplasty, breast augmentation and, yes, liposuction.
The cost of health care of the entire pool would rise dramatically, causing premiums to rise for everyone in that insurance pool. To prevent this from happening, insurance companies are only willing to cover procedures that they, under the advisement of medical doctors, find medically necessary.
There are some loopholes that may permit liposuction to be covered by insurance. There are some instances, for example, of liposuction being covered as a part of another procedure. Liposuction is generally a part of breast reduction surgery, for example, which is often deemed medically necessary to reduce pressure, pain, and risk of injury to the spinal cord. This liposuction would be covered by some insurance companies if they approve the procedure overall.
There are other conditions for which liposuction may be considered therapeutic. The presence of lipomas, or fatty tumors, is one such condition. Lipomas can cause discomfort and, rarely, become carcinogenic. In the case of cancerous lipomas, surgical excision or liposuction may be approved by an insurance company, Medicaid or Medicare as a course of treatment.
There are also cases where insurance covers liposuction if the fat removed is used to graft another part of the body, such as the breasts in the case of breast reconstruction or face in the case of facial reconstruction.
Frequently Asked Questions About Insurance and Liposuction

– Is liposuction considered medically necessary if it will help my back?
Unfortunately, liposuction is not among the approved treatments for back pain. Back pain and other joint and skeletal pain can be ameliorated with weight loss, but liposuction is not considered a weight loss procedure like bariatric surgeries are.
As previously mentioned, liposuction’s main purpose is to spot reduce fat in individuals who are otherwise a healthy weight.
Keep in mind that policies on cosmetic procedures used as therapies vary by insurance company and some may be more liberal than others. If you are considering liposuction in the near future, it is worth calling different companies in an attempt to find the one whose policies best fit your goals.
– Why is a gastric sleeve and/or gastric bypass covered by my insurance, but not liposuction?

Liposuction is categorized by insurance companies as a cosmetic procedure. Bariatric procedures like gastric banding, gastric sleeve, gastric bypass and duodenal switch, on the other hand, are categorized as weight loss surgeries and approved obesity therapies.
Much research, deliberation, and the establishment of practice standards factors into what is considered an approved therapy by the medical community. Because obesity is such a multifactorial and complicated disease, it is even more difficult to determine what counts as a treatment. In fact, some nutrition and exercise services, long accepted as the first-line therapies for the treatment and prevention of obesity, are not covered by many insurance companies.
Another reason bariatric surgery is covered is that these procedures often reduce the severity of, and sometimes even cure, obesity-related comorbidities such as heart disease, diabetes, insulin resistance or pre-diabetes, hypertension and obstructive sleep apnea. Liposuction does not have such a dramatic effect on chronic disease. This means it is not as simple to justify coverage by insurance companies.
– What options are available to pay for liposuction if insurance denies my claim?

For individuals who still feel like liposuction is the right choice for them and their goals, there are some options available. A patient’s plastic surgeon can provide contact information for financing companies who allow patients to pay for their surgeries in installments over time. Some doctors’ offices may also allow direct financing.
How Can I Find Out More About Insurance and Liposuction
Your insurance company is the best resource when it comes to coverage and benefits. Patients can consult their Explanation of Benefits, received monthly or quarterly from their insurance companies.
If these documents are difficult to interpret or fail to explicitly state the companies policies on cosmetic procedures used as therapies, patients are encouraged to call the customer service line.
In the end, insurance companies approve claims on a case-by-case basis. If a surgeon or primary care physician drafts a letter or makes a few phone calls defending the therapeutic benefit of liposuction for that particular patient, it can sway insurance companies to consider the procedure a reconstructive procedure or therapy. Keep in mind that surgeons are professionals, and will only recommend liposuction as a reimbursable therapy if it truly is.
No reputable surgeon will call the insurance company for a cosmetic procedure on your behalf. Surgeons understand the reasoning behind insurance’s failure to cover cosmetic procedures.
Click here to compare coverage from various providers in your state today!
- http://www.health.harvard.edu/staying-healthy/abdominal-fat-and-what-to-do-about-it
- http://www.aetna.com/cpb/medical/data/1_99/0031.html
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2884718/
- https://www.hindawi.com/journals/psi/2015/625396/
- http://www.breastcancer.org/treatment/surgery/reconstruction/types/autologous/fat-grafting